Contents
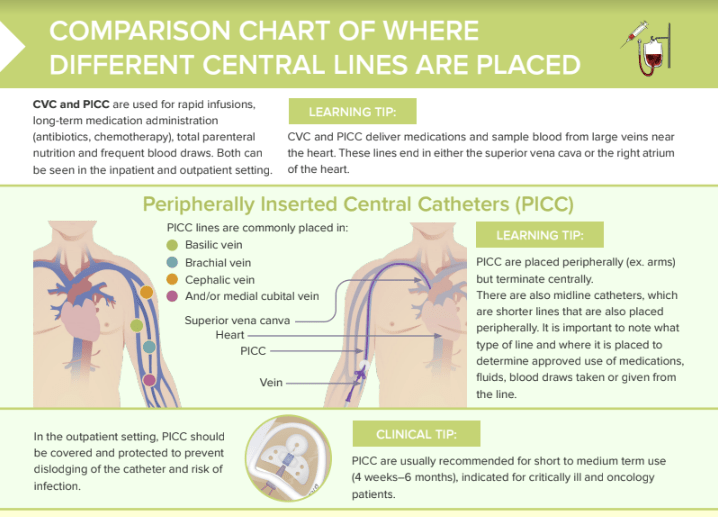
Why Use A Picc Line Over A Central Line Advantages And Considerations Midline catheter. according to infusion nurses society, midline catheter is defined as a vascular access device which is inserted into a peripheral vein (namely, basilic, cephalic, or brachial vein), and the tip of it is at or near axilla level, and distal to the shoulder. the midline catheters can remain in situ up to 30 days. A peripherally inserted central catheter (picc) is a small flexible tube that is inserted into a vein on the inside of your upper arm. a picc extends into the large central vein that returns blood to your heart. the catheter does not go into your heart. with a picc, medicines, fluids, and nutrients can be given directly into your vein.
Midline Vs Picc Line Difference And Comparison All neonate nicu infusions, including central line flushes, should be administered using a pump to reduce the risk of catheter fracture. after completion of any infusion or blood sampling, or every 6 hours. heparin 10units ml; flush with 1ml (10units) piccs and power injectable piccs (e.g. bard power picc) all neonate nicu infusions, including. Understanding the diverse central vascular access options available to nurses is paramount for ensuring effective patient care delivery. these access devices play a critical role in delivering medications and fluids, and obtaining blood samples, particularly in patients requiring long term intravenous therapy. given the multitude of options: picc line vs central line vs midline, nurses must […]. A picc may be inserted at the bedside by several practitioners or a radiologist who may opt for fluoroscopic guidance to ensure intraoperative safety and correct catheter positioning. a picc is a 50 cm to 60 cm long catheter with up to 3 lumens, most commonly placed into a peripheral vein in the arm and terminates in proximity to the cavoatrial. Generally, 8 25cm long, midline catheters are inserted with ultrasound guidance into the larger diameter veins of the upper arm and tend to last longer than a piv. the cdc states to use a midline catheter or picc instead of a short peripheral catheter if the duration of iv therapy will likely exceed six days (o’grady et al., 2011).

Midlines Vs Picc Lines Etsy A picc may be inserted at the bedside by several practitioners or a radiologist who may opt for fluoroscopic guidance to ensure intraoperative safety and correct catheter positioning. a picc is a 50 cm to 60 cm long catheter with up to 3 lumens, most commonly placed into a peripheral vein in the arm and terminates in proximity to the cavoatrial. Generally, 8 25cm long, midline catheters are inserted with ultrasound guidance into the larger diameter veins of the upper arm and tend to last longer than a piv. the cdc states to use a midline catheter or picc instead of a short peripheral catheter if the duration of iv therapy will likely exceed six days (o’grady et al., 2011). The median (iqr) age of device recipients was 64.8 (53.4 75.4) years for both picc and midline patients, and 5741 (52.8%) were female. both picc and midline recipients had similar comorbidity burden (median charlson score = 3 for both cohorts). single lumen devices represented 63.2% of piccs and 84.9% of midlines. A: by definition, the difference is: picc is short for peripherally inserted central catheter. it is a central vascular access device inserted into an extremity and advanced in the venous system until the distal tip is positioned in the vena cava. midline (ml) catheter is a vascular access device measuring 8 inches or less with the distal tip.
